Mild traumatic brain injury cases turn on proof. A client who walked away from a rear-end crash, scored a 15 on the Glasgow Coma Scale, and showed a clean head CT can still finish the year unable to follow a recipe or hold the schedule that paid the mortgage. The hard part is making the injury visible to a jury under Oklahoma’s evidence rules.
This page is the procedural companion to our overview of mild TBI litigation challenges. It walks through the proof steps that carry weight in Oklahoma County and Cleveland County district courts: imaging that survives a Daubert motion, a neuropsychological battery a defense expert cannot wave away, the paid-not-incurred rule in 12 O.S. § 3009.1, life-care planning, vocational analysis, and lay testimony. The trial lawyers at Hasbrook & Hasbrook Personal Injury Lawyers build cases through each of these stages.
The defense playbook is consistent: a normal head CT becomes “no objective injury,” self-reported memory symptoms become “subjective complaints,” and a return-to-work date becomes “full recovery.” The jury hears “mild” and discounts everything after. The CDC estimates roughly 15 percent of mild TBIs produce symptoms lasting more than a year, and the Brain Injury Association of America calls mild TBI the most under-diagnosed injury in trauma medicine. A CT scan looks for bleeds and skull fractures, not the diffuse axonal shearing that drives most concussion symptoms.
Building admissible imaging: DTI, SWI, and the Daubert hurdle
Diffusion tensor imaging (DTI) and susceptibility-weighted imaging (SWI) are the MRI sequences that detect microstructural damage a normal CT misses. DTI maps white-matter tract integrity using fractional anisotropy values; SWI shows microbleeds invisible to standard sequences. The American Association of Neurological Surgeons recognizes both as advanced TBI imaging, and peer-reviewed literature on NIH Bookshelf describes DTI as the most sensitive method for axonal injury after closed head trauma. The fight is whether the jury gets to see it.
The 12 O.S. § 2702 expert standard
Oklahoma adopted the federal Daubert framework through 12 O.S. § 2702. A neuroradiologist offering DTI testimony must show the opinion rests on sufficient facts, reliable principles, and methods reliably applied. Defense counsel almost always moves in limine to exclude DTI as research-only science. The motion does not always succeed, but it always gets filed.
What survives a Daubert challenge in our experience:
- An MRI ordered through a treating neurologist with a documented clinical indication, not litigation-driven imaging at a freestanding outpatient facility
- A radiologist who reads the study clinically and produces a written report, not an expert retained only to interpret a scan months later
- Comparison to the patient’s own pre-injury baseline where available, or to age-matched normative atlases where it is not
- A peer-reviewed methodology cited in the radiology report, with replication-rate data when the defense asks
What does not survive: a DTI report from a vendor marketing directly to plaintiffs’ lawyers, with no treating relationship and no clinical correlation. The court excludes it, and the defense uses the exclusion against the rest of the case.
The neuropsychological battery: what gets weight, what gets thrown out
Imaging shows the brain; neuropsychological testing shows the deficit. A skilled neuropsychologist administers standardized tests scored against age-and-education-matched norms and produces a written report tying deficits to the mechanism of injury.
The batteries that consistently carry weight in Oklahoma district courts are anchored on:
- WAIS-IV for processing speed, working memory, and overall cognitive index. A working-memory score 1.5 standard deviations below the verbal-comprehension score is the classic mild-TBI fingerprint.
- RBANS for serial measurement across appointments, useful for documenting non-recovery
- Trail Making Test A and B for divided attention and executive function
- California Verbal Learning Test (CVLT-II) for verbal memory encoding and retrieval
- Embedded validity measures (Test of Memory Malingering, Word Memory Test) so the defense cannot allege effort failure
The validity measures are not optional. A report without documented effort testing is the report the defense uses to argue exaggeration; a report with passing scores on three or more validity measures forecloses that argument.
Treating versus retained
Where the testing happens matters as much as the testing itself. A neuropsychologist the patient saw on a treating-physician referral, with insurance billing and chart notes, reads to a jury as part of the medical record. A neuropsychologist hired by counsel three weeks before trial reads as a paid witness. We aim for the first track on every mild TBI file we accept.
Medical bills under 12 O.S. § 3009.1: paid, not incurred
Oklahoma is a paid-not-incurred state. Under 12 O.S. § 3009.1, the only medical bills admissible at trial are amounts actually paid by or for the plaintiff, plus amounts still owed after insurance write-offs. The chargemaster sticker price never reaches the jury.
For a mild TBI client the math is brutal. A $14,000 brain MRI might post an $1,800 paid amount after insurance write-offs. The jury sees $1,800, and the defense uses the small number to argue the injury was small. Three procedural moves matter:
- Pre-trial motion to clarify what counts as “paid.” Health insurance write-offs are excluded; Med Pay and UIM payments are not, under the collateral source doctrine that operates inside § 3009.1’s narrow exception.
- Lien-driven future-cost evidence. Future neurology visits, repeat imaging, and ongoing neuropsychological re-testing are not yet “paid” and come in through expert testimony on reasonable future medical expense.
- Treating-physician testimony on reasonableness. A treating neurologist can testify that the billed amounts were reasonable and necessary even when the paid amount differs. This frames the paid number as a billing artifact, not a measure of injury severity.
Our workflow for clients with significant write-offs is mapped in the attorney-side billing-evidence flowchart we use at deposition.
Statute of limitations
The two-year clock under 12 O.S. § 95 runs from the date of injury, not diagnosis. Mild TBI symptoms often emerge in the second or third week, but the limitations period does not pause.
The life-care planner’s role
A certified life-care planner converts a treating neurologist’s prognosis into a year-by-year cost projection. For post-concussive syndrome that lingers past 18 months, the plan typically captures:
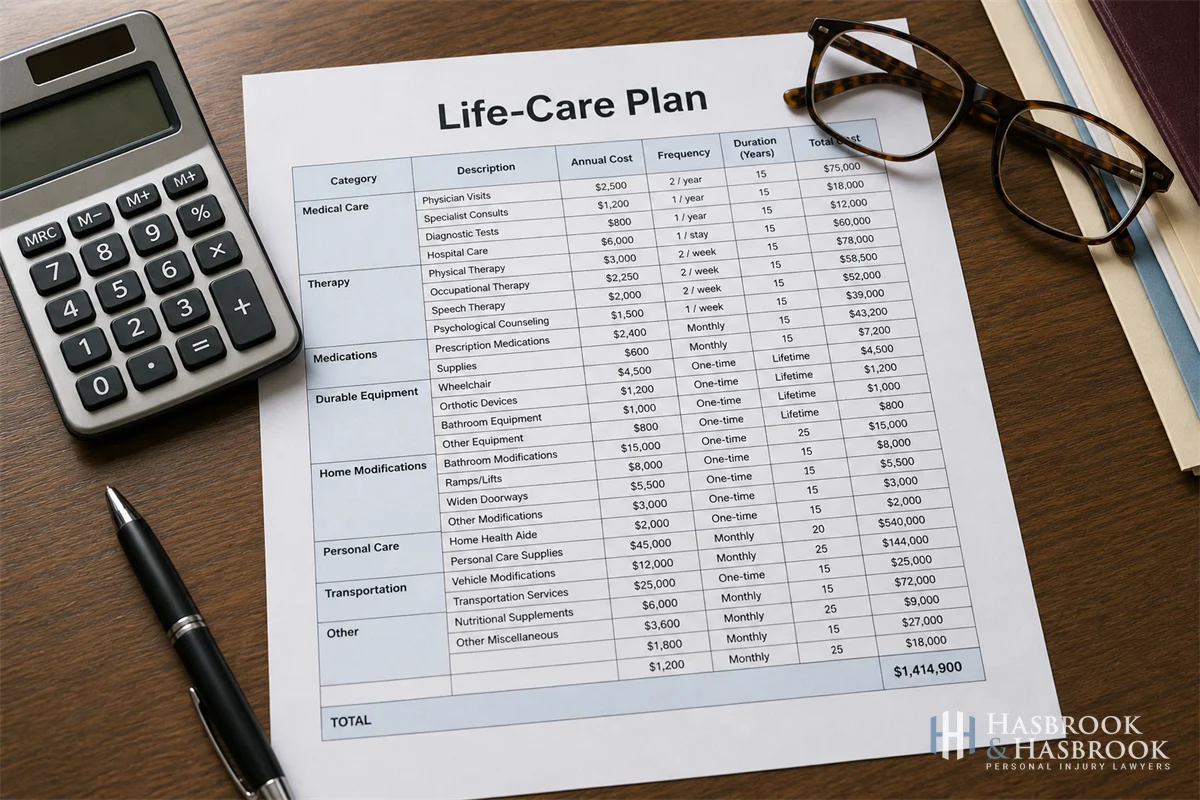
- Annual neurology follow-up and repeat imaging at defined intervals
- Cognitive rehabilitation therapy (speech-language pathology, occupational therapy)
- Pharmacology for headache, sleep regulation, and mood stabilization
- Psychiatric or counseling support for adjustment-related depression and anxiety
- Vocational rehabilitation when earning capacity has declined
- Adaptive technology (calendaring software, voice-to-text, memory aids)
The plan must be built from treating providers’ written orders, not generic CDC averages. A plan that cites a treating physician on every line is an exhibit; a plan built from internet research is something the defense picks apart at deposition. See our life-care planning practice, future medical costs, and adaptive equipment.
The vocational expert: linking deficit to lost earning capacity
Lost wages are easy. Lost earning capacity is the harder claim and the larger one. A vocational expert reviews the neuropsych battery, treating providers’ restrictions, pre-injury job duties, and the local labor market, and opines on what the client can realistically earn going forward. Vocational testimony for a mild TBI plaintiff usually documents:
- Pre-injury job description with measurable cognitive demands (multitasking, deadline density, novel-problem-solving frequency)
- Post-injury restrictions translated from the neuropsych report (e.g., processing speed at the 15th percentile rules out positions requiring rapid client-facing decisions)
- Specific Oklahoma-market wage differential between the pre-injury position and any reasonable replacement work
- Worklife-expectancy reduction backed by Department of Labor data, projected to retirement age
For clients whose careers required cognitive flexibility (commercial driving, nursing, teaching, sales, skilled-trades supervision), vocational damages often exceed every other category combined. See loss of earning capacity for the analytical framework.
Video diaries: the day-in-the-life evidence the defense plays down
A mild TBI client looks normal on deposition video; the same client struggling to follow a three-step morning routine looks injured. A contemporaneous video diary is the cheapest, most powerful piece of evidence in a mild-TBI file.

What we ask clients to record, starting within the first month after the crash:
- Two-minute clips of routine tasks (cooking, reading mail, paying a bill online, homework help) with timestamps
- The same task repeated every two weeks across the first six months, so the jury sees the trajectory
- Spontaneous symptom episodes (headache onset, vertigo, word-finding lapses) when the client thinks to capture them
- Family member voiceover only with client authorization; never staged or scripted
The video must read as documentary, not produced. We do not coach what the client says; we coach the format. Phone propped on a counter, single take, no editing. Defense counsel can attack a polished day-in-the-life film, but a 90-second clip of a parent missing a step in a familiar recipe is harder to dismiss.
Lay witness testimony from family and coworkers
Under the Oklahoma Evidence Code, a family member, friend, or coworker can testify to observable changes in the plaintiff’s behavior, personality, and functioning without being qualified as an expert. This “before-and-after” testimony does work no expert can replicate.
The value comes from specificity. “He’s not himself anymore” is weak. “She coached our daughter’s softball team for six years and quit after the wreck because she could not track three batters in a row” is strong. Our intake captures these witnesses at the first client meeting, and we depose them in chief on our schedule.
A useful structure for direct examination of a spouse or longtime coworker:
- Establish the relationship and its duration before the injury
- Describe two or three specific routines or projects the witness observed pre-injury
- Describe the same routines after the injury, with dates and concrete examples
- Confirm the absence of confounders (no prior cognitive decline, substance issues, or separate health events)
- Close with the witness’s most recent observation, dated within 90 days
Putting the proof package together
| Element | Provider | Document or output | Procedural anchor |
|---|---|---|---|
| Microstructural injury imaging | Treating neuroradiologist | DTI / SWI written report | 12 O.S. § 2702 admissibility |
| Cognitive deficit measurement | Neuropsychologist (treating) | WAIS-IV, RBANS, validity-measure scores | Standardized norms, embedded effort tests |
| Past medical billing | Treating providers and billing custodians | Paid-amount affidavits | 12 O.S. § 3009.1 |
| Future care projection | Certified life-care planner | Year-by-year cost plan | Treating-physician orders on each line |
| Lost earning capacity | Vocational expert | Wage-differential and worklife report | Department of Labor data, OK-market wages |
| Day-to-day functioning | Client and family | Video diary clips | Lay observation, contemporaneous |
| Personality and routine change | Spouse, coworker, longtime friend | Lay testimony at deposition and trial | Oklahoma Evidence Code lay opinion |
Defense IME preparation
The defense will request an independent medical exam, usually with an expert who consistently testifies for insurers. Our pre-IME protocol is in our IME guide and the defense medical exam protocol. Three points for mild TBI plaintiffs: request the defense expert’s prior testimony list and IME billing through interrogatories, bring a court reporter where practice permits, and produce records only through formal discovery.
Damages, comparative fault, and the cap
Economic damages (medical expenses paid, future medical care, lost wages, lost earning capacity) are uncapped under Oklahoma law. Noneconomic damages face a $500,000 cap under 23 O.S. § 61.3 effective September 2025; the cap has not been tested at the Oklahoma Supreme Court since the prior cap was struck down in Beason v. I.E. Miller Services, Inc., 2019 OK 28. Whether the new statute clears the same constitutional bar is an open question. We file noneconomic claims fully and preserve the constitutional challenge in the alternative.
Comparative fault is often disputed. Oklahoma’s modified rule under 23 O.S. § 13 reduces recovery by the plaintiff’s share and bars recovery only when the plaintiff’s fault exceeds the defendant’s. At exactly half fault, the plaintiff still recovers. A clean DTI study and a clean neuropsychological battery shift the jury’s focus from impact magnitude to demonstrable injury, which is friendlier ground for the plaintiff. See how the 50% bar applies when both drivers share blame, pain-and-suffering calculation, and punitive damages eligibility for related categories.

Settlement timing and when to bring in counsel
Settling a mild TBI claim before the neuropsychological battery is finished is the most common way clients leave money on the table. Symptoms often peak at three to six months, plateau at twelve to eighteen, and reach a measurable baseline near the two-year mark. An offer in month four anchors the claim to incomplete medicine. We do not engage serious settlement until the treating neuropsychologist has documented either a return to baseline or a stable floor across two repeat batteries six months apart. Companion reading: mild-to-moderate TBI recovery, cognitive testing after a brain injury, and the TBI valuation overview.
Mild TBI cases resolve well when a lawyer is involved before the first neuroimaging decision. Once a defense IME is calendared without a treating neuropsychologist of record, the case is harder to rebuild. We accept mild TBI cases on contingency, advance imaging and expert costs, and commit to producing a record that holds up at trial. Call (405) 605-2426 or use the contact form.
Frequently asked questions
Does a normal head CT mean I do not have a brain injury?
No. A normal CT rules out bleeding and skull fracture. It does not rule out diffuse axonal injury, the most common mechanism in mild TBI. DTI and SWI are designed to detect what CT cannot.
How long do I have to file a mild TBI lawsuit in Oklahoma?
Two years from the date of injury under 12 O.S. § 95. The clock does not pause because symptoms emerged later. File before the deadline even if treatment is ongoing.
Will the jury see what my hospital billed, or only what insurance paid?
Only the paid amount is admissible under 12 O.S. § 3009.1, plus any unpaid balance. A treating physician can testify to reasonableness of the billed charges.
What if I was partially at fault for the crash?
You can still recover under 23 O.S. § 13 as long as your fault does not exceed the defendant’s. Recovery is reduced by your percentage. At exactly half fault, you still recover a reduced amount.
How much does a neuropsychological evaluation cost?
A full battery typically runs $2,500 to $6,500 in Oklahoma. With health insurance, the treating-track exam is usually covered by referral. Where insurance does not cover it, our firm advances the cost as a litigation expense.
Can my spouse or coworker testify about my brain injury?
Yes. Lay witnesses can describe observable changes in your behavior, routines, and abilities without being qualified as experts.












