Oklahoma’s “paid versus incurred” rule decides which medical-bill numbers a jury sees in your personal injury trial. The dollar figure you pay out of pocket, the dollar figure your provider billed, and the dollar figure your health insurer paid are often three very different numbers. 12 O.S. § 3009.1 tells the trial court which of those numbers is admissible as evidence of medical damages. Get the rule wrong and a $100,000 hospital bill can shrink to a $14,000 evidentiary number before the jury ever hears about it.
At Hasbrook & Hasbrook Personal Injury Lawyers, we file every Oklahoma case with the § 3009.1 framework already mapped onto the medical billing record. This page walks through the statute, the appellate decisions that survived constitutional challenge, the Oklahoma Bar Association ethics opinion on lien preparation, and the practical math your case turns on.
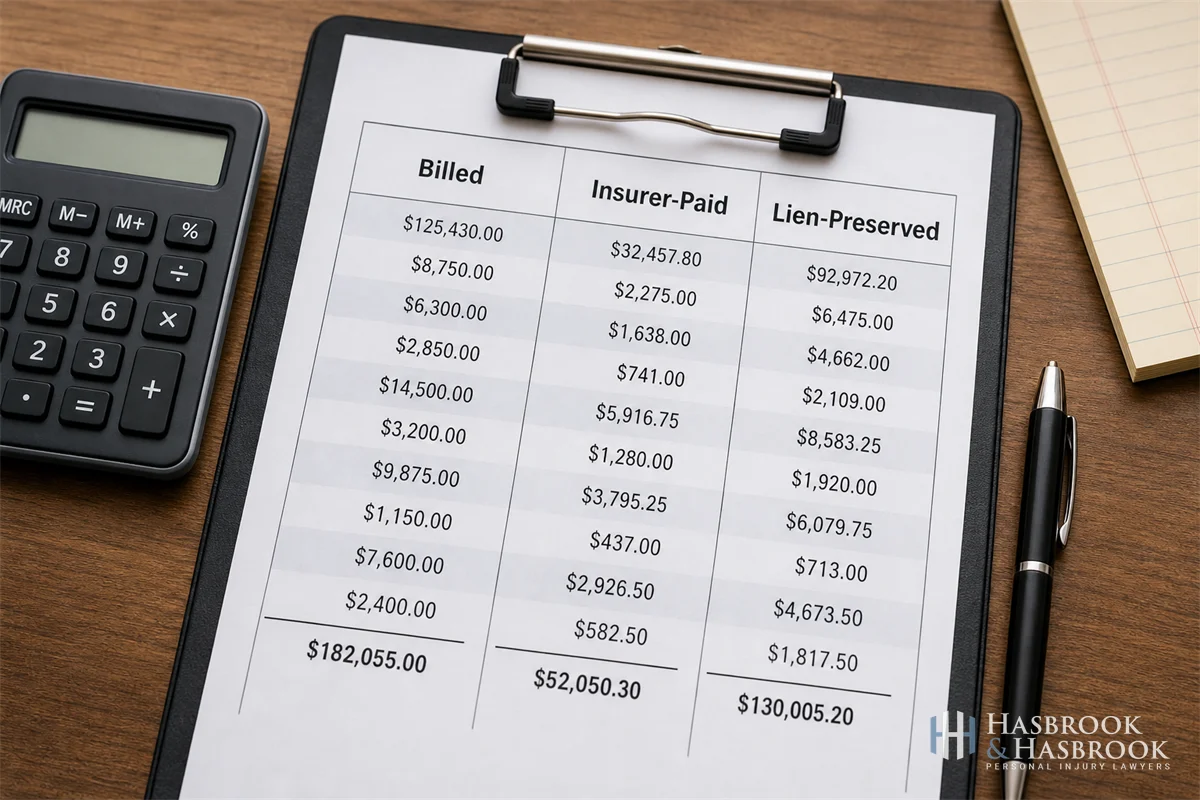
How § 3009.1 Decides Which Medical-Bill Number Reaches the Jury
Before the statute took effect, Oklahoma followed the traditional collateral-source rule, which kept defendants from benefiting when somebody else (a health insurer, Medicare, or SoonerCare) paid the plaintiff’s medical bills. Section 3009.1 changed that. The statute reads in plain terms but the four scenarios it creates need to be sequenced carefully.
The four-tier admissibility ladder under § 3009.1:
- Tier 1 (bills paid in full). The actual amount paid is admissible, not the amount originally billed. A statement from the provider accepting that amount as full payment is also admissible.
- Tier 2 (no payment yet, but provider verifies a Medicare-rate cap). If the provider signs off that it would accept the Medicare reimbursement rate in effect at the time of injury as full payment, that rate is admissible instead of the billed amount.
- Tier 3 (no payment, no rate verification). The original billed amount is admissible.
- Tier 4 (a statutory lien exceeds the paid or Medicare-rate amount). The amount up to the lien value is admissible, even if higher than the paid amount.
Tiers 1 and 2 are where most defense leverage lives. Tier 4 is where careful lien work can recapture value the statute would otherwise strip out of the case. Our internal tier-by-tier admissibility flowchart we use during exhibit prep walks through each fork before billing exhibits are designated.
What Real Numbers Look Like Under the Statute
The starkest illustration of § 3009.1 is comparing identical injuries with different payor mixes:
| Scenario | Billed | Health Plan / Source | Amount Paid | Admissible Number |
|---|---|---|---|---|
| Commercial PPO (BCBS / Cigna) | $25,000 | BlueCross BlueShield | $10,000 | $10,000 |
| Medicaid (SoonerCare) | $25,000 | SoonerCare | $5,000 | $5,000 |
| Uninsured / self-pay | $25,000 | None | $0 | $25,000 (subject to lien tier) |
| Med-pay only | $25,000 | Auto med-pay | $5,000 (then exhausted) | $5,000 + balance under tier rules |
Three plaintiffs with identical injuries and identical providers walk into court with three different damages numbers. That outcome is the statutory design, not a glitch. The Insurance Information Institute’s primer on auto-coverage tiers explains why payor mix varies so widely on the same fact pattern. Most clients do not realize how much of their case value rides on a billing-office line item until we lay the math out side by side. The same dynamic shapes our analysis on the variables that drive case-value modeling and on whether medical bills are paid out of a car accident settlement.
Health-plan write-offs do not vanish. The plan keeps a right of subrogation, which means it usually has to be paid back from any settlement. Whether that reimbursement is full, reduced, or waived depends on the plan type (ERISA self-funded, fully insured, Medicare, or Medicaid) and on the negotiation. Our overview of subrogation in personal injury cases covers the discount levers; for federal payors specifically, the Medicare-Medicaid lien resolution checklist tracks the pre-settlement steps. If your treatment is still ongoing, see also our notes on why MMI changes the timing of a settlement decision and on recovering out-of-pocket expenses that the statute does not touch.
The Four Oklahoma Supreme Court Decisions That Locked In § 3009.1
Section 3009.1 has been challenged repeatedly. The Oklahoma Supreme Court has consistently upheld the statute and clarified its scope.
- Gowens v. Barstow (2015 OK 85). The Court applied § 3009.1 to limit medical-expense evidence to amounts actually paid but expressly declined to decide whether Medicaid write-offs qualify as a collateral source. That open question is still live in trial-court practice.
- Lee v. Bueno (2016 OK 95). The Court held § 3009.1 is constitutional. It limits the form of medical-cost evidence but does not deny access to the courts and does not violate due process. The opinion reasoned the statute does not abolish the collateral-source rule, but controls evidentiary rules where they conflict.
- Christian v. Lee (2016). The Court applied Lee v. Bueno to reverse a trial-court ruling that § 3009.1 was unconstitutional. After Christian, trial-level constitutional attacks on the statute stopped being viable.
- Hill v. American Medical Response (2018 OK 57). The Court held the statute does not violate due process or unlawfully delegate legislative authority by referencing the AMA Guides for permanent-impairment evaluation.
The takeaway: the statute is the rule, the constitutional fight is over, and trial work has to happen inside the four tiers above. The full text of § 3009.1 on Justia is worth keeping on the case file for cross-examination of records custodians.
Medical Liens, Right-to-Receive Payment, and OBA Ethics Opinion 329
Tier 4 turns on whether a hospital, physician, or related provider has a perfected lien that exceeds the paid amount. Oklahoma’s hospital lien is at 42 O.S. § 43; the medical-services lien is at 42 O.S. § 46. A provider that knows it will accept less than the billed amount can still preserve a lien for the full billed amount, which can keep evidentiary value above what the insurer paid.
That intersection produced an ethics question: can a plaintiff’s attorney ethically prepare a lien for the client’s medical providers? The Oklahoma Bar Association answered in Ethics Opinion No. 329.
OBA Opinion 329 holds:
- Concurrent representation of the injured client and the provider is permitted under Oklahoma Rule of Professional Conduct 1.7 only when (a) the lawyer reasonably believes competent representation is possible, (b) the matter is not legally prohibited, (c) the claims are not directly adverse, and (d) both clients give informed written consent.
- Solicitation letters to providers are allowed as advertising under Rules 7.2 and 7.3, but cannot involve coercion, duress, or harassment, and cannot be motivated primarily by pecuniary gain in a way that crosses the rule against direct in-person solicitation.
- The lawyer must explain the conflict risk to both sides before taking on the lien preparation.
- The lawyer should not charge the provider a fee for preparing the lien, except for actual filing costs.
Practically, our firm tracks the full lien posture before designating bills as exhibits, because a lien filed late or defectively can collapse a Tier 4 case back into Tier 1 numbers. The tracker we maintain for perfecting and validating provider liens is the document we use to keep that record straight, and the Oklahoma lien-priority rules reference covers competing claims (hospital vs. health-plan vs. attorney’s lien under FindLaw’s general framework on medical bills and injury claims). For background on why a treating doctor’s office may file a lien in the first place, see our explainer on why a doctor’s office files a lien.
What This Means for Your Oklahoma Personal Injury Case

If you are weighing a settlement or preparing for trial, the § 3009.1 checklist looks like this:
- Pull every itemized bill, every Explanation of Benefits, and every payment ledger from each provider.
- Identify the payor on each line and tag it as commercial, Medicare, Medicaid, med-pay, workers’ compensation, or self-pay.
- Confirm whether a lien has been filed or can still be perfected before trial.
- Calculate the admissible number under the four tiers; flag the gap between billed and admissible.
- Build the closing-argument story that explains why the admissible number understates the actual harm without contradicting the statute.
The math is unforgiving. So is the deadline. A separate piece walks through the two-year statute of limitations for personal injury claims in Oklahoma, which controls when the lawsuit must be filed. Before signing anything from an adjuster, see our companion guides on how carriers value bills line by line during pre-suit negotiation, post-accident strategies with adjusters, and what to do when the other driver lacks adequate coverage. Documentation matters: the records you collect are what feed the four-tier analysis, and our walkthrough on how to document injuries for a personal injury claim covers the basics. To weigh a settlement number, compare what we see across different injury types in pieces like when a case is worth more than the insurance policy and whether the offer is fair. If a public entity is involved, the rules shift again under the Governmental Tort Claims Act, walked through on our GTCA notice and damages-cap walkthrough page; for cases outside the metro, see our Ardmore personal injury lawyer location page.
Our firm has built personal injury cases in Oklahoma across two generations. our managing attorney handles the trial-evidence framework on every file in the office. If your medical bills, lien posture, and payor mix have been thrown at you with a blank settlement number on top, call our office at (405) 605-2426 for a no-cost case review. We will tell you what the admissible damages number really looks like before you decide what to do next.











